Managing your finances on a fixed income leaves very little room for error. When utility bills, housing costs, and food prices rise, your monthly budget tightens. One of the most stressful expenses you face in retirement is the cost of medications. Skipping doses or cutting pills in half to save money puts your health at serious risk, yet thousands of retirees make this dangerous compromise every day because they simply cannot afford their pharmacy bills.
You do not have to choose between buying groceries and filling your prescriptions. The federal and state governments offer multiple assistance programs designed specifically to lower or completely eliminate medication costs for older adults. Many seniors assume they do not qualify because they own a home or have a small savings account; however, eligibility rules are much broader than you might think.
Understanding which programs apply to your specific financial situation can unlock thousands of dollars in annual savings. By taking advantage of these government resources, you can stabilize your retirement budget and secure the medications you need to stay healthy.

The Reality of Prescription Costs on a Fixed Income
Healthcare is consistently one of the largest expenses in retirement. Even with Medicare Part D covering a portion of your drug costs, deductibles, premiums, and copayments can drain your monthly cash flow quickly. When you rely solely on Social Security or a modest pension, an unexpected diagnosis requiring expensive brand-name drugs can instantly derail your financial stability.
To understand the profound impact of prescription assistance, look at how a typical senior’s budget changes when they successfully apply for government aid. The table below illustrates a hypothetical monthly budget for a single senior with an income of $1,800 per month, comparing their expenses before and after enrolling in programs like Medicare Extra Help and a Medicare Savings Program.
| Monthly Budget Category | Without Assistance | With Government Assistance |
|---|---|---|
| Income | $1,800 | $1,800 |
| Housing & Utilities | $950 | $950 |
| Food & Groceries | $300 | $300 |
| Medicare Part B Premium | $174.70 | $0 (Covered by MSP) |
| Prescription Copays & Premiums | $250 | $25 (Capped by Extra Help) |
| Remaining Cash Flow | $125.30 | $500.00 |
As the table demonstrates, removing the burden of Medicare premiums and high prescription copays frees up nearly $400 a month. This extra cash provides an essential buffer for emergencies, home repairs, or simply enjoying a higher quality of life. Let us look at the specific programs that make this financial relief possible.
Program 1: Medicare Extra Help (The Low-Income Subsidy)
If you have Medicare Part D, the Extra Help program is the single most powerful tool available to lower your out-of-pocket medication costs. According to the Social Security Administration (SSA), this program provides an estimated $5,300 in value each year to seniors who qualify.
Recent changes under the Inflation Reduction Act have expanded this program significantly. Previously, seniors had to navigate a complex system of partial subsidies based on exact income brackets. Now, the program offers full benefits to anyone who meets the income and asset limits. If you qualify, your Medicare Part D monthly premium vanishes, your annual deductible is eliminated, and your pharmacy copayments are strictly capped at just a few dollars per prescription—typically around $4.50 for generic drugs and $11.20 for brand-name medications.
Eligibility Guidelines:
- You must reside in one of the 50 states or the District of Columbia.
- Your combined savings, investments, and real estate (excluding your primary home, vehicles, and personal possessions) must fall below the federal asset limits.
- Your annual income must fall below the threshold, though limits are slightly higher for married couples living together.
Even if your income is slightly above the official limit, you should still apply. Certain portions of your income, such as assistance you receive from family members to pay household bills, may not be counted during the evaluation process.

Program 2: Medicaid Coverage for Seniors
Medicaid is a joint federal and state program that provides comprehensive health coverage to individuals with limited income and resources. When a senior qualifies for both Medicare and Medicaid, they are known as “dual eligible.”
If you become dual eligible, Medicaid acts as a secondary insurance that picks up the costs Medicare leaves behind. Most importantly, qualifying for Medicaid automatically enrolls you in the Medicare Extra Help program discussed above. Medicaid also frequently covers medications, vitamins, and over-the-counter drugs that are entirely excluded from Medicare Part D formularies.
Because Medicaid is administered at the state level, the income and asset rules vary depending on where you live. Some states have “medically needy” pathways; this means if your income is technically too high for Medicaid, but you have massive medical bills that consume most of your money, the state allows you to subtract those medical expenses from your income to qualify.

Program 3: Qualified Medicare Beneficiary (QMB) Program
The QMB program is one of four Medicare Savings Programs (MSPs) managed by your state. While it is primarily known for paying your Medicare Part A and Part B premiums, its impact on your prescription drug costs is indirect but massive.
First, the QMB program pays your Part B premium (which is over $170 a month for most seniors), putting that money directly back into your checking account to pay for daily living expenses. Second, federal law prohibits any medical provider who accepts Medicare from billing QMB participants for Medicare deductibles, coinsurance, or copayments. Finally, just like Medicaid, enrolling in the QMB program automatically qualifies you for Extra Help for your prescriptions.
For a senior surviving on $1,200 a month from Social Security, removing premium deductions and capping prescription costs through QMB completely transforms their financial outlook.

Program 4: Specified Low-Income Medicare Beneficiary (SLMB)
If your income is slightly too high to qualify for the QMB program, you may still qualify for the SLMB program. This program has higher income limits but serves a similar foundational purpose: it pays your Medicare Part B premium.
While the SLMB program does not cover your Medicare deductibles or coinsurance like QMB does, it still automatically grants you full enrollment into the Medicare Extra Help program. This means that by qualifying for SLMB, you instantly bypass the normal Extra Help application process and lock in those rock-bottom $4.50 and $11.20 copay maximums at the pharmacy counter.

Program 5: Qualifying Individual (QI) Program
The QI program is the third major Medicare Savings Program, designed for seniors whose incomes are slightly higher than the SLMB limits. Like SLMB, the QI program pays your Part B premium and automatically enrolls you in the Extra Help prescription drug program.
There is one crucial difference with the QI program: it operates on a first-come, first-served basis. The federal government gives each state a limited amount of money to fund the QI program each year. Once the state runs out of funding, no further applications are approved, regardless of whether you meet the financial criteria. If you suspect you fall into this income bracket, it is imperative to apply early in the calendar year to secure your spot.
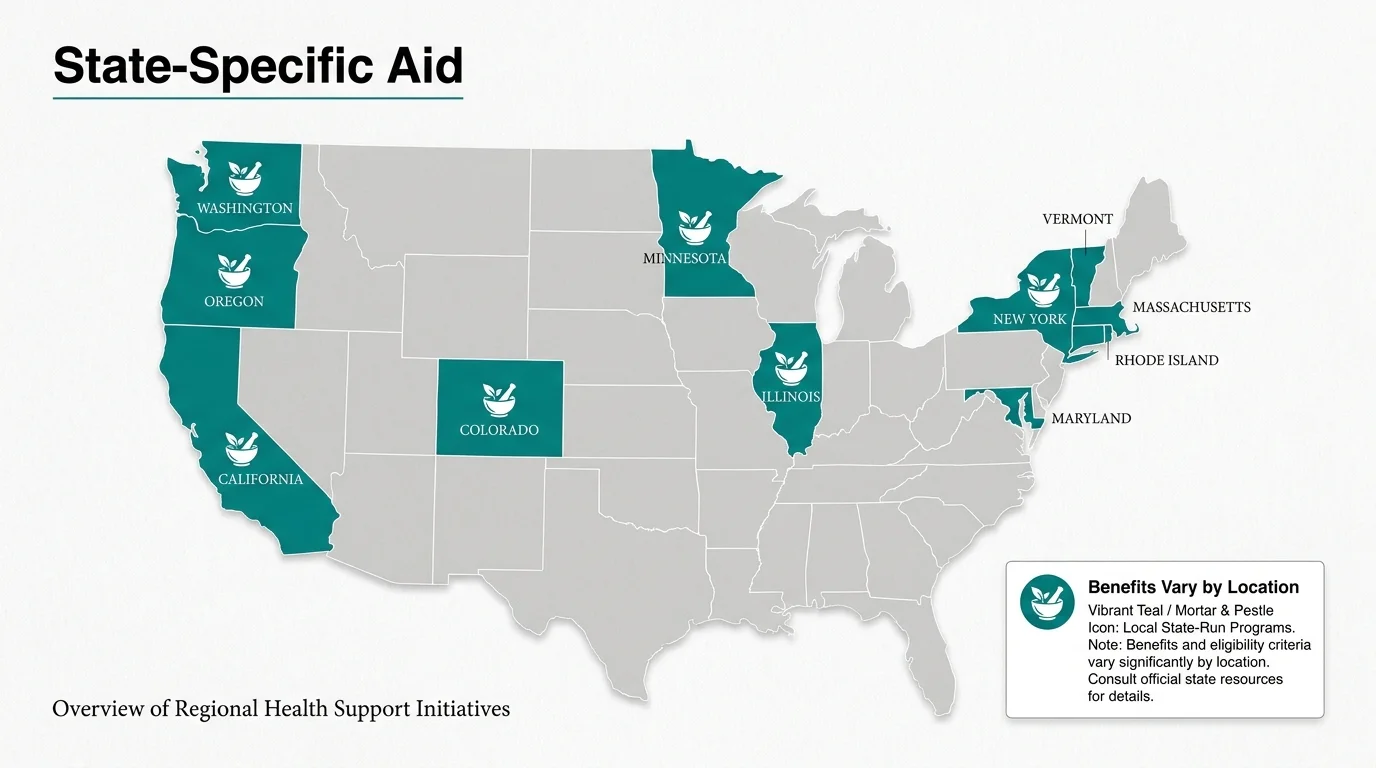
Program 6: State Pharmaceutical Assistance Programs (SPAPs)
Not all help comes directly from the federal government. Many state governments have created their own programs to help seniors pay for medications. State Pharmaceutical Assistance Programs (SPAPs) are explicitly designed to wrap around your Medicare Part D coverage.
Depending on your state, an SPAP might pay your Part D monthly premium, cover your copays at the pharmacy, or pay for drugs during your coverage gap. Because these programs are funded by individual states, the benefits and eligibility requirements vary wildly. For instance, New York’s Elderly Pharmaceutical Insurance Coverage (EPIC) program and Pennsylvania’s PACE/PACENET programs are highly generous, offering robust coverage to hundreds of thousands of residents.
To find out if your state offers an SPAP and what the specific income limits are, the Eldercare Locator is an excellent starting point. Simply enter your ZIP code or city to connect with your local Area Agency on Aging, which maintains updated lists of state-specific drug benefits.

Program 7: Program of All-Inclusive Care for the Elderly (PACE)
PACE is a unique, comprehensive Medicare and Medicaid program designed to help vulnerable seniors stay in their communities rather than moving into a nursing home. If you require a nursing home level of care but can live safely at home with support, PACE provides a complete team of healthcare professionals to manage your medical needs.
When you join PACE, you receive all your Medicare and Medicaid benefits—including all prescription drugs—through the program. If you are eligible for Medicaid, you will generally not pay a monthly premium for the long-term care portion of the PACE benefit, and you will have zero copayments for any medications approved by your PACE healthcare team.
To qualify for PACE, you must be 55 or older, live in the service area of a PACE organization, and be certified by your state as needing a nursing home level of care.

Program 8: Veterans Affairs (VA) Pharmacy Benefits
If you are a veteran of the U.S. Armed Forces, you may have access to one of the most cost-effective pharmacy programs in the country. The VA provides prescription medications to enrolled veterans, often at a fraction of the cost of retail pharmacies.
VA prescription benefits operate on a tier system. Depending on your priority group—which is determined by factors like your income and whether you have service-connected disabilities—you may receive your medications completely free of charge. For others, the maximum copay for a 30-day supply of a tiered medication rarely exceeds $24, which is significantly cheaper than many Medicare Part D copays for specialty drugs.
You are allowed to have both VA health care and Medicare Part D. Many savvy veterans use their VA benefits to get their expensive maintenance medications through the mail at low cost, while keeping a basic Part D plan to fill urgent, short-term prescriptions (like antibiotics) at their local neighborhood pharmacy.

Program 9: Community Health Centers (340B Program)
The federal government provides grants to Community Health Centers (also known as Federally Qualified Health Centers, or FQHCs) to serve populations with limited access to healthcare. Through a federal initiative called the 340B Drug Pricing Program, these clinics purchase medications from pharmaceutical companies at steeply discounted rates.
When you become a patient at an FQHC, they pass these discounts directly on to you. They use a sliding fee scale based entirely on your current income, regardless of your insurance status. If your income is very low, you might pay only a nominal fee—such as $5 or $10—for an expensive medication that would normally cost hundreds of dollars.
You can discover local federally funded health clinics and other broad assistance initiatives by utilizing resources from Benefits.gov, which provides a comprehensive benefit finder tool customized to your specific needs.
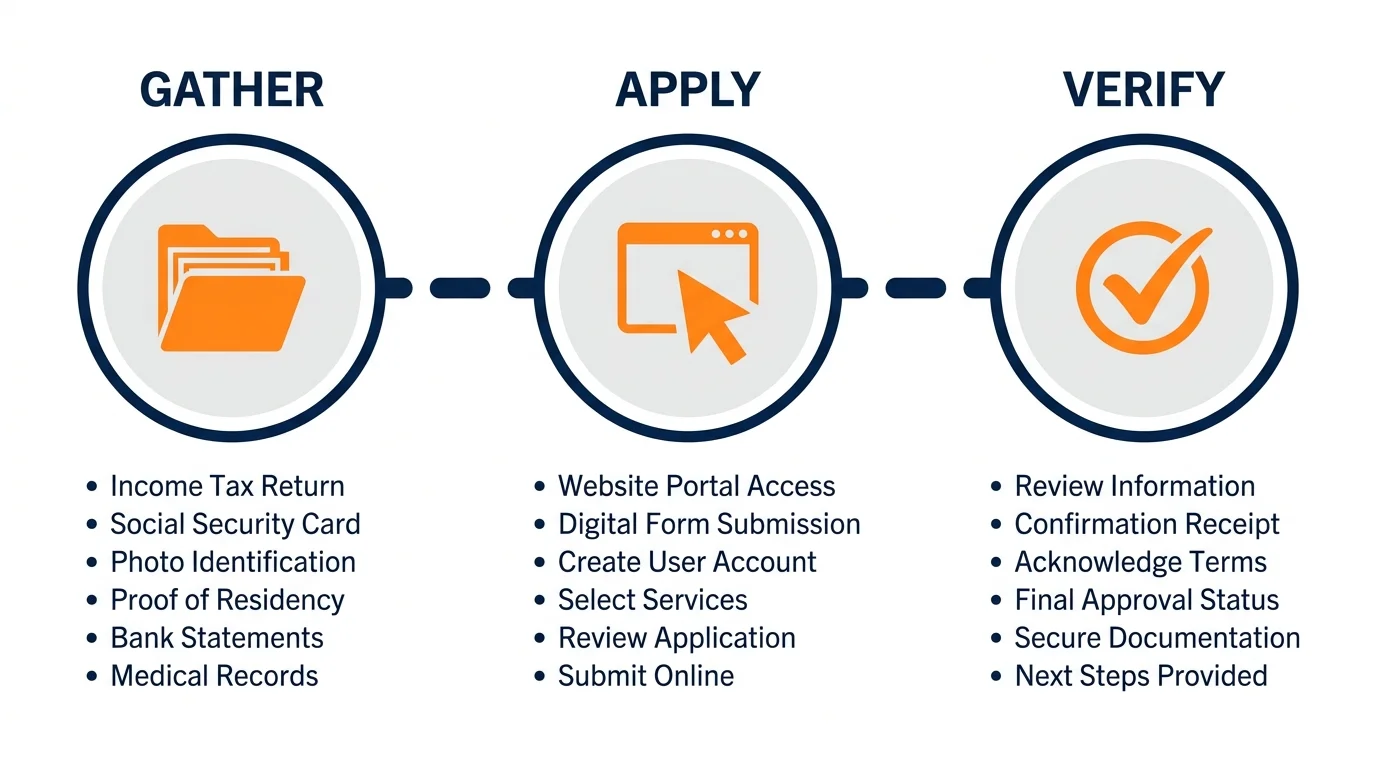
How to Apply and Verify Your Eligibility
Navigating the bureaucracy of government programs can feel overwhelming. However, applying for these programs usually requires the same basic set of documents. Gathering your financial information before you start will save you hours of frustration.
Your Application Checklist:
- Your Medicare card and Social Security card.
- Recent bank statements (checking and savings accounts) for the last three months.
- Proof of your current income, such as your annual Social Security award letter, pension statements, or annuity documents.
- Statements for any investments, including IRAs, 401(k)s, stocks, or mutual funds.
- A complete list of your current medications and the dosages.
You can apply for the Medicare Extra Help program directly online through the Social Security website. The application takes about 15 minutes, and you do not need to upload physical documents; you simply self-report your numbers, which the government verifies against tax records. For Medicaid and Medicare Savings Programs, you must apply through your state’s local Medicaid office or Department of Social Services.
To double-check how these programs will integrate with your specific Part D plan, you can verify your coverage options using resources from Medicare.gov. Their online tools allow you to input your exact drug list to see how much you will pay at local pharmacies under different subsidy scenarios.

Avoiding Prescription Discount Scams
Unfortunately, the complexity of prescription pricing makes seniors prime targets for fraud. Criminals know that retirees are anxious about healthcare costs and exploit this fear using high-pressure tactics.
Data from the Consumer Financial Protection Bureau (CFPB) shows that seniors frequently lose money and risk identity theft through sophisticated healthcare scams. Be highly suspicious of anyone who calls you out of the blue offering “free government prescription cards” or demanding your Medicare number to “verify your new benefits.”
Protect yourself with these rules:
- The government will never call you unprompted to ask for your Medicare number, Social Security number, or bank details.
- Legitimate government programs (like Extra Help or Medicaid) are entirely free to apply for. If a company asks for an “application fee” or “processing fee” to get you enrolled in a prescription program, it is a scam.
- Be wary of fake discount cards sold online. While there are legitimate commercial discount programs (like GoodRx), you should never have to pay a monthly membership fee to an unknown company just to access standard pharmacy discounts.
Frequently Asked Questions
Do these government programs cover vitamins and dietary supplements?
Generally, Medicare Part D and Extra Help do not cover over-the-counter vitamins, supplements, or weight-loss drugs. However, if you qualify for full Medicaid, your state may cover certain doctor-prescribed vitamins (like prescription-strength Vitamin D) if they are deemed medically necessary. Always check your specific state’s Medicaid formulary.
Can I use VA pharmacy benefits if I already have Medicare Part D?
Yes; you are allowed to have both. However, they do not coordinate or merge. If you fill a prescription at a VA pharmacy, you use your VA benefits. If you go to a local retail pharmacy (like Walgreens or CVS), you must use your Medicare Part D card. You cannot use your Part D plan to pay for VA copays, nor can you use the VA to pay for Part D copays.
Does my house or car count as an asset when applying for Extra Help?
No. The federal government specifically excludes your primary residence, your personal vehicles, your household furnishings, and personal jewelry when calculating your assets for the Extra Help program. They are primarily looking at liquid assets: cash, bank accounts, stocks, bonds, and real estate other than your primary home.
What happens if I apply for a Medicare Savings Program but my income fluctuates?
Eligibility for Medicare Savings Programs is generally reviewed once a year during a recertification process. If your income fluctuates slightly month-to-month, it usually will not cause immediate cancellation. However, if you experience a permanent, significant change in income (such as starting to draw from an inherited IRA), you are required to report this to your state’s Medicaid office, which could affect your eligibility for the following year.
Will Extra Help pay for a drug if it is not on my Medicare plan’s formulary?
No. Extra Help lowers the costs of the drugs that your Part D plan already covers. If a medication is not on your plan’s formulary, Extra Help will not pay for it. In this scenario, you and your doctor must file an exception request with your Medicare plan to get the drug covered. Once the plan approves the exception, your Extra Help benefits will kick in to lower the copay.
For official financial guidance for seniors, visit
Centers for Medicare & Medicaid Services (CMS), Consumer Financial Protection Bureau (CFPB), IRS.gov, Benefits.gov and AARP.
Disclaimer: This article is for informational purposes and is not a substitute for professional financial or tax advice. Consult with a certified financial planner or tax professional for guidance on your specific situation.











Leave a Reply